Overview
This Guidelines summary provides recommendations on assessing the risk of fragility fractures in primary care. Included are recommendations on targeting risk assessment and using different methods of assessment.
Infographic Summary
- The Institute of Osteopathy has produced a visual guide to the NICE guideline on osteoporosis.
Algorithm 1: Fragility Fracture Risk Assessment in People Aged 18 and Over with Osteoporosis
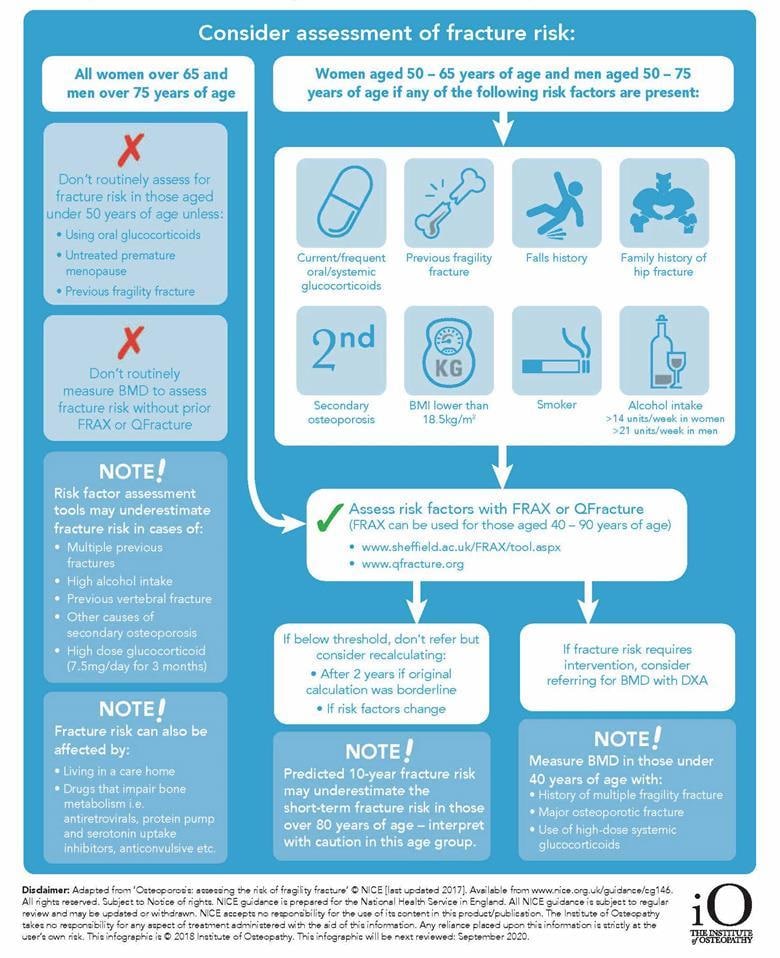
Targeting Risk Assessment
- Consider assessment of fracture risk:
- In all women aged 65 years and over and all men aged 75 years and over
- in women aged under 65 years and men aged under 75 years in the presence of risk factors, for example:
- previous fragility fracture
- current use or frequent recent use of oral or systemic glucocorticoids
- history of falls
- family history of hip fracture
- other causes of secondary osteoporosis[A]
- low body mass index (BMI) (less than 18.5 kg/m2)
- smoking
- alcohol intake of more than 14 units per week for men and women.
- Do not routinely assess fracture risk in people aged under 50 years unless they have major risk factors (for example, current or frequent recent use of oral or systemic glucocorticoids, untreated premature menopause or previous fragility fracture), because they are unlikely to be at high risk.
Methods of Risk Assessment
- Estimate absolute risk when assessing risk of fracture (for example, the predicted risk of major osteoporotic or hip fracture over 10 years, expressed as a percentage).
- Use either FRAX[B] (without a bone mineral density [BMD] value if a dual-energy X-ray absorptiometry [DXA] scan has not previously been undertaken) or QFracture[C], within their allowed age ranges, to estimate 10-year predicted absolute fracture risk when assessing risk of fracture. Above the upper age limits defined by the tools, consider people to be at high risk.
- Interpret the estimated absolute risk of fracture in people aged over 80 years with caution, because predicted 10-year fracture risk may underestimate their short-term fracture risk.
- Do not routinely measure BMD to assess fracture risk without prior assessment using FRAX (without a BMD value) or QFracture.
- Following risk assessment with FRAX (without a BMD value) or QFracture, consider measuring BMD with DXA in people whose fracture risk is in the region of an intervention threshold[D] for a proposed treatment, and recalculate absolute risk using FRAX with the BMD value.
- Consider measuring BMD with DXA before starting treatments that may have a rapid adverse effect on bone density (for example, sex hormone deprivation for treatment for breast or prostate cancer).
- Measure BMD to assess fracture risk in people aged under 40 years who have a major risk factor, such as history of multiple fragility fracture, major osteoporotic fracture, or current or recent use of high-dose oral or high-dose systemic glucocorticoids (more than 7.5 mg prednisolone or equivalent per day for 3 months or longer).
- Consider recalculating fracture risk in the future:
- if the original calculated risk was in the region of the intervention threshold[E] for a proposed treatment and only after a minimum of 2 years, or
- when there has been a change in the person’s risk factors.
- Take into account that risk assessment tools may underestimate fracture risk in certain circumstances, for example if a person:
- has a history of multiple fractures
- has had previous vertebral fracture(s)
- has a high alcohol intake
- is taking high-dose oral or high-dose systemic glucocorticoids (more than 7.5 mg prednisolone or equivalent per day for 3 months or longer)
- has other causes of secondary osteoporosis.[A]
- Take into account that fracture risk can be affected by factors that may not be included in the risk tool, for example living in a care home or taking drugs that may impair bone metabolism (such as anti-convulsants, selective serotonin reuptake inhibitors, thiazolidinediones, proton pump inhibitors and anti-retroviral drugs).
Footnotes
[A] Causes of secondary osteoporosis include endocrine (hypogonadism in either sex including untreated premature menopause and treatment with aromatase inhibitors or androgen deprivation therapy; hyperthyroidism; hyperparathyroidism; hyperprolactinaemia; Cushing's disease; diabetes), gastrointestinal (coeliac disease; inflammatory bowel disease; chronic liver disease; chronic pancreatitis; other causes of malabsorption), rheumatological (rheumatoid arthritis; other inflammatory arthropathies), haematological (multiple myeloma; haemoglobinopathies; systemic mastocytosis), respiratory (cystic fibrosis; chronic obstructive pulmonary disease), metabolic (homocystinuria), chronic renal disease and immobility (due for example to neurological injury or disease).
[B] FRAX can be used for people aged between 40 and 90 years, either with or without BMD values, as specified.
[C] QFracture can be used for people aged between 30 and 84 years. BMD values cannot be incorporated into the risk algorithm.
[D] An intervention threshold is the level of risk at which an intervention is recommended. People whose risk is in the region from just below to just above the threshold may be reclassified if BMD is added to assessment. It is out of the scope of this guideline to recommend intervention thresholds. Healthcare professionals should follow local protocols or other national guidelines for advice on intervention thresholds.
[E] An intervention threshold is the level of risk at which an intervention is recommended. It is out of the scope of this guideline to recommend intervention thresholds. Healthcare professionals should follow local protocols or other national guidelines for advice on intervention thresholds.

